The Morse Fall Scale is a widely used assessment tool in healthcare settings to evaluate a patient's risk of falling. Developed by Dr. Mary Morse, this scale helps healthcare professionals identify patients who are at a higher risk of falls, allowing for timely interventions to prevent injuries. Understanding and effectively using the Morse Fall Scale can significantly improve patient safety and outcomes.
Understanding the Morse Fall Scale
The Morse Fall Scale is designed to assess six key factors that contribute to a patient's fall risk. These factors include:
- History of falling
- Secondary diagnosis
- Ambulatory aid
- I.V. or heparin lock
- Gait
- Mental status
Each factor is assigned a score, and the total score determines the patient's fall risk category. The scale ranges from 0 to 125, with higher scores indicating a greater risk of falling.
Components of the Morse Fall Scale
The Morse Fall Scale evaluates the following components:
History of Falling
This component assesses whether the patient has a history of falling. A history of falls is a strong predictor of future falls. The scoring for this component is as follows:
- No history of falling: 0 points
- History of falling: 25 points
Secondary Diagnosis
Secondary diagnoses that increase the risk of falling include conditions such as neurological disorders, orthopedic impairments, and metabolic disorders. The scoring for this component is:
- No secondary diagnosis: 0 points
- Secondary diagnosis: 15 points
Ambulatory Aid
The use of ambulatory aids, such as walkers or canes, can indicate a higher risk of falling. The scoring for this component is:
- No ambulatory aid: 0 points
- Uses ambulatory aid: 15 points
I.V. or Heparin Lock
The presence of an intravenous (I.V.) line or heparin lock can increase the risk of falling due to the limitations it imposes on the patient's mobility. The scoring for this component is:
- No I.V. or heparin lock: 0 points
- I.V. or heparin lock: 20 points
Gait
Gait assessment evaluates the patient's ability to walk. A normal gait is scored lower, while an impaired gait is scored higher. The scoring for this component is:
- Normal gait: 0 points
- Weak gait: 10 points
- Impaired gait: 20 points
Mental Status
Mental status assessment includes evaluating the patient's cognitive function and orientation. A normal mental status is scored lower, while an impaired mental status is scored higher. The scoring for this component is:
- Normal mental status: 0 points
- Mildly impaired mental status: 15 points
- Moderately to severely impaired mental status: 30 points
Scoring and Interpretation
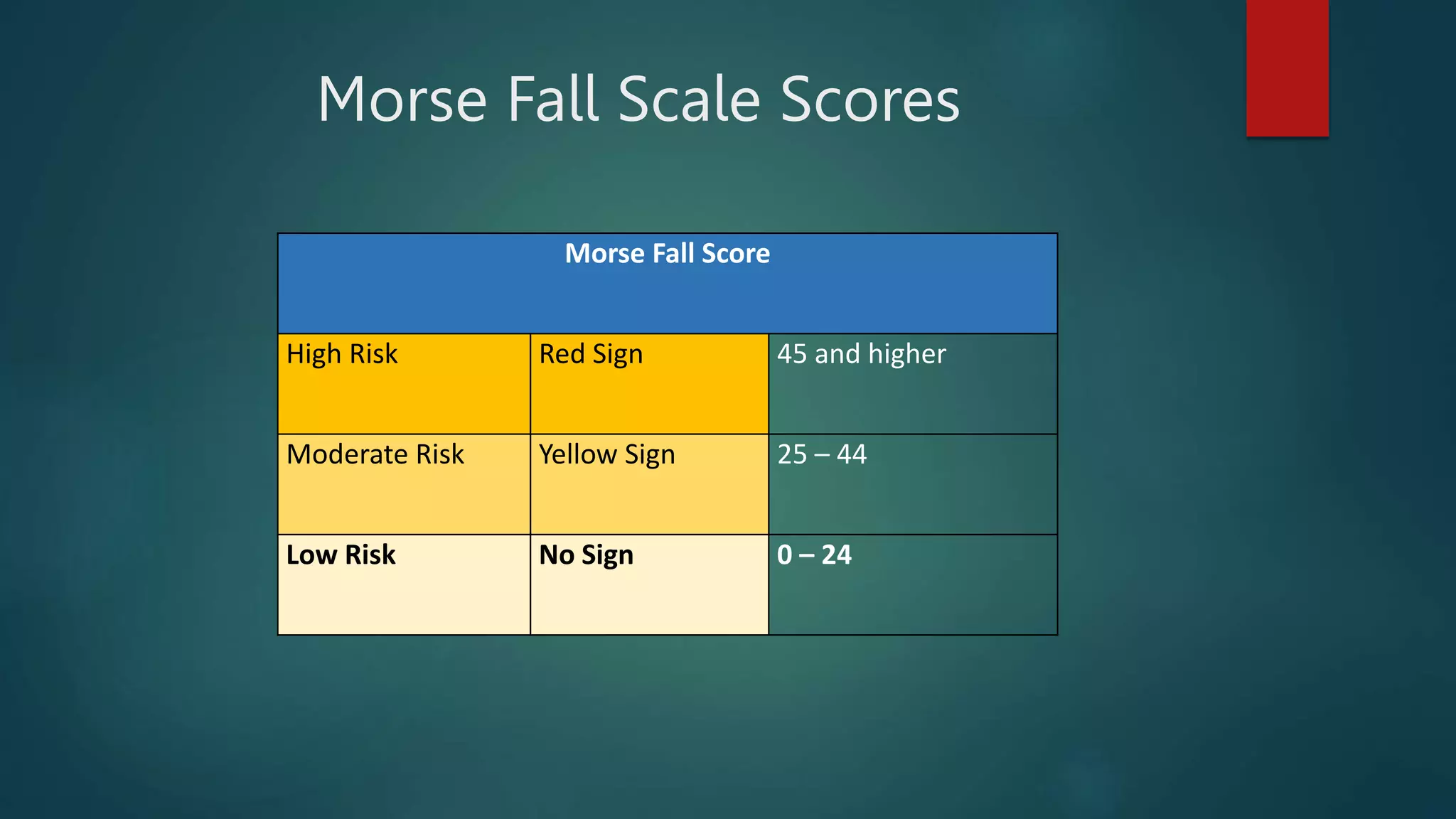
The total score from the Morse Fall Scale is used to categorize the patient's fall risk. The categories and their corresponding scores are as follows:
| Fall Risk Category | Score Range |
|---|---|
| Low Risk | 0-24 |
| Medium Risk | 25-50 |
| High Risk | 51 and above |
Patients with a score of 0-24 are considered low risk, those with a score of 25-50 are considered medium risk, and those with a score of 51 and above are considered high risk. This categorization helps healthcare professionals determine the appropriate interventions and precautions to take.
Implementing the Morse Fall Scale
Implementing the Morse Fall Scale in a healthcare setting involves several steps:
Training Staff
Ensure that all healthcare staff are trained on how to use the Morse Fall Scale. This includes understanding the components of the scale, how to assess each factor, and how to interpret the scores. Regular training sessions and updates can help maintain consistency and accuracy in fall risk assessments.
Conducting Assessments
Conduct regular fall risk assessments using the Morse Fall Scale for all patients. This should be done upon admission and at regular intervals during the patient's stay. The assessments should be documented in the patient's medical record for reference and continuity of care.
Interpreting Results
Interpret the results of the Morse Fall Scale to determine the patient's fall risk category. Based on the category, implement appropriate interventions and precautions to prevent falls. For example, patients at high risk may require closer monitoring, assistive devices, and environmental modifications.
Documenting and Communicating
Document the fall risk assessment results in the patient's medical record. Communicate the findings to all relevant healthcare team members to ensure a coordinated approach to fall prevention. Clear communication helps in implementing consistent interventions and precautions.
📝 Note: Regular updates and reviews of the fall risk assessment are crucial, especially for patients with changing health conditions.
Interventions for Fall Prevention
Based on the Morse Fall Scale results, various interventions can be implemented to prevent falls. These interventions are tailored to the patient's specific risk factors and fall risk category. Some common interventions include:
Environmental Modifications
Modify the patient's environment to reduce fall risks. This may include:
- Removing clutter and obstacles from the patient's room
- Ensuring adequate lighting
- Installing grab bars and handrails
- Using non-slip mats and flooring
Assistive Devices
Provide assistive devices to help patients with mobility issues. This may include:
- Walkers and canes
- Wheelchairs
- Bed alarms and chair alarms
Patient Education
Educate patients and their families about fall prevention strategies. This may include:
- Teaching patients how to safely transfer from bed to chair
- Instructing patients on the proper use of assistive devices
- Encouraging patients to call for help when needed
Monitoring and Supervision
Provide close monitoring and supervision for patients at high risk of falling. This may include:
- Regular check-ins by healthcare staff
- Using bed and chair alarms
- Assigning a dedicated caregiver
Challenges and Limitations
While the Morse Fall Scale is a valuable tool for assessing fall risk, it is not without its challenges and limitations. Some of the key challenges include:
Subjectivity in Assessment
The assessment of certain components, such as gait and mental status, can be subjective and may vary between healthcare providers. This subjectivity can lead to inconsistencies in scoring and interpretation.
Dynamic Nature of Patient Conditions
Patient conditions can change rapidly, and a single assessment may not capture the dynamic nature of fall risk. Regular reassessments are necessary to ensure accurate and up-to-date fall risk evaluations.
Resource Constraints
Implementing fall prevention interventions can be resource-intensive, requiring additional staff, equipment, and environmental modifications. Healthcare settings with limited resources may face challenges in providing comprehensive fall prevention measures.
📝 Note: Regular training and updates for healthcare staff can help mitigate the subjectivity in assessments and ensure consistency in fall risk evaluations.
Case Studies and Best Practices
Several case studies and best practices highlight the effective use of the Morse Fall Scale in various healthcare settings. These examples demonstrate how the scale can be integrated into daily practice to improve patient safety and outcomes.
Case Study: Acute Care Hospital
In an acute care hospital, the Morse Fall Scale was implemented as part of the admission process. All patients were assessed upon admission, and their fall risk category was documented in their medical records. Based on the assessment results, appropriate interventions were implemented, such as environmental modifications, assistive devices, and increased monitoring. The hospital reported a significant reduction in fall-related injuries within six months of implementing the scale.
Best Practice: Long-Term Care Facility
In a long-term care facility, regular fall risk assessments using the Morse Fall Scale were conducted for all residents. The facility trained its staff on the scale and ensured consistent documentation and communication of fall risk assessments. Residents at high risk were provided with assistive devices and environmental modifications. The facility also implemented a fall prevention education program for residents and their families. This comprehensive approach resulted in a 30% reduction in fall incidents over a year.
Future Directions
The Morse Fall Scale continues to be a valuable tool in fall risk assessment, but there is always room for improvement. Future directions in fall prevention may include:
Technological Advancements
Incorporating technological advancements, such as wearable devices and smart sensors, can enhance fall risk assessments and interventions. These technologies can provide real-time monitoring and alerts, improving the accuracy and timeliness of fall prevention measures.
Integrated Fall Prevention Programs
Developing integrated fall prevention programs that combine the Morse Fall Scale with other assessment tools and interventions can provide a more comprehensive approach to fall prevention. These programs can include multidisciplinary teams, patient education, and environmental modifications.
Research and Evidence-Based Practices
Continuing research and evidence-based practices can help refine the Morse Fall Scale and improve its effectiveness. Studies on the scale's validity, reliability, and applicability in different healthcare settings can provide valuable insights and recommendations for future use.
In conclusion, the Morse Fall Scale is a crucial tool for assessing and managing fall risk in healthcare settings. By understanding the components of the scale, conducting regular assessments, and implementing appropriate interventions, healthcare professionals can significantly reduce the incidence of falls and improve patient safety. The scale’s effectiveness is enhanced through consistent training, documentation, and communication, ensuring that fall prevention measures are tailored to each patient’s unique needs. As healthcare continues to evolve, the Morse Fall Scale will remain a cornerstone in fall risk assessment, guiding best practices and improving patient outcomes.
Related Terms:
- morse fall scale chart
- morse fall scale score
- original morse fall scale
- morse fall scale printable
- morse fall scale interpretation
- morse fall risk assessment