Epidermolysis Bullosa (EB) is a rare genetic disorder that affects the skin and mucous membranes, causing them to be extremely fragile and prone to blistering. This condition can significantly impact the quality of life and, in some cases, the Epidermolysis Bullosa age expectancy. Understanding the various types of EB, their symptoms, and the available treatments is crucial for managing this condition effectively.
Understanding Epidermolysis Bullosa
Epidermolysis Bullosa is characterized by the skin's inability to withstand mechanical stress, leading to blistering and erosion. The severity of EB can vary widely, ranging from mild to life-threatening. The condition is typically classified into four main types:
- Epidermolysis Bullosa Simplex (EBS): This is the most common and generally the mildest form of EB. It primarily affects the skin and can cause blisters on the hands and feet.
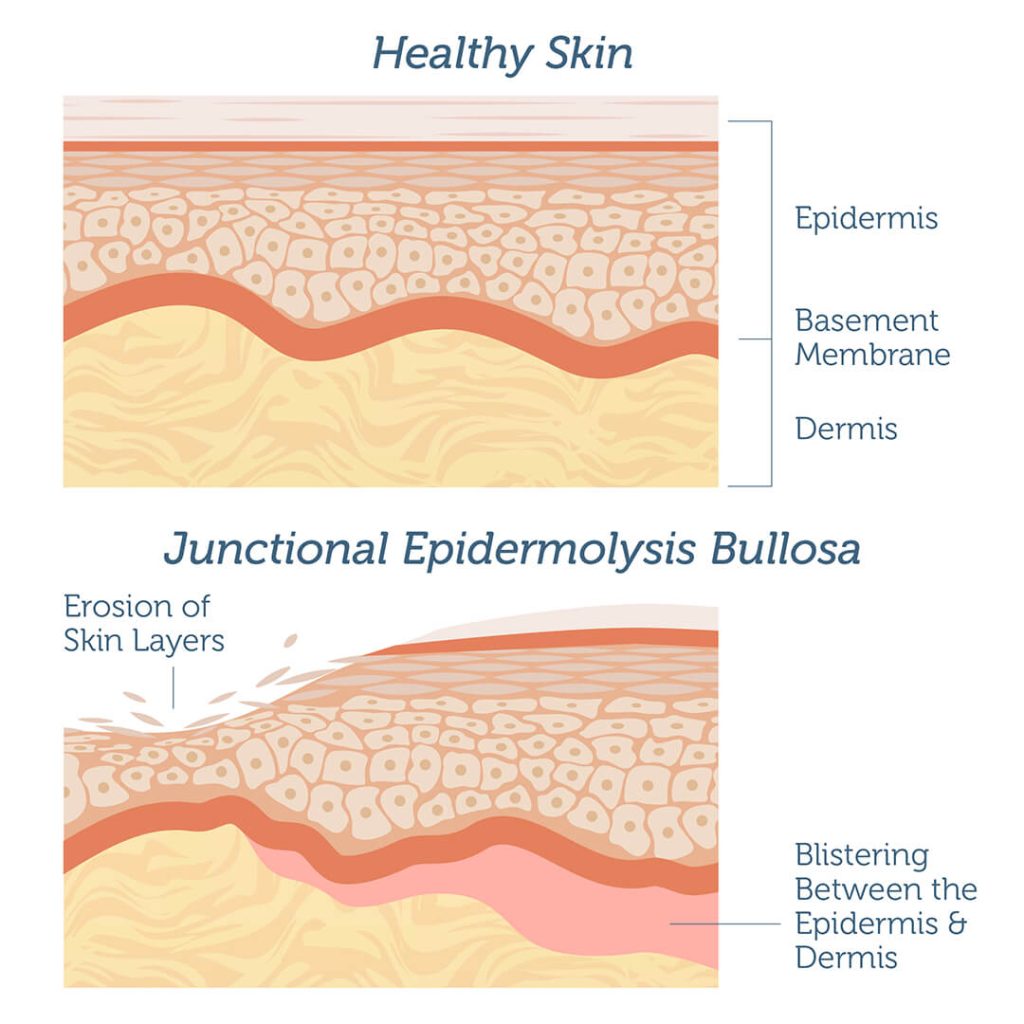
- Junctional Epidermolysis Bullosa (JEB): This type is more severe and can affect both the skin and internal organs. It often results in significant scarring and can be life-threatening.
- Dystrophic Epidermolysis Bullosa (DEB): This form can be either dominant or recessive. The recessive form is particularly severe and can lead to extensive scarring and deformities.
- Kindler Syndrome: This is a rare form of EB that combines features of other types. It can cause blistering, photosensitivity, and progressive skin changes.
Symptoms of Epidermolysis Bullosa
The symptoms of EB can vary depending on the type and severity of the condition. Common symptoms include:
- Blistering and erosion of the skin, often triggered by minor trauma.
- Scarring and deformities, particularly in severe forms.
- Nail abnormalities, including ridging, thickening, and loss of nails.
- Oral and esophageal blistering, which can make eating difficult.
- Internal blistering, which can affect the digestive tract, respiratory system, and other organs.
Diagnosing Epidermolysis Bullosa
Diagnosing EB involves a combination of clinical evaluation, genetic testing, and skin biopsy. The diagnostic process typically includes:
- Physical examination to assess the extent and severity of skin blistering and erosion.
- Genetic testing to identify mutations in the genes associated with EB.
- Skin biopsy to examine the layers of the skin and determine the type of EB.
- Immunofluorescence mapping to visualize the proteins involved in skin adhesion.
Treatment Options for Epidermolysis Bullosa
While there is no cure for EB, various treatments can help manage symptoms and improve the quality of life. Treatment options include:
- Wound Care: Regular and meticulous wound care is essential to prevent infections and promote healing. This may involve the use of non-adhesive dressings, topical antibiotics, and pain management.
- Pain Management: Chronic pain is a common issue for individuals with EB. Pain management strategies may include oral medications, topical anesthetics, and alternative therapies like acupuncture.
- Nutritional Support: Proper nutrition is crucial for healing and overall health. A balanced diet, along with nutritional supplements, can help support the body's healing processes.
- Physical Therapy: Physical therapy can help maintain mobility and prevent contractures, which are common in severe forms of EB.
- Surgical Interventions: In some cases, surgery may be necessary to correct deformities, release contractures, or manage complications like esophageal strictures.
Epidermolysis Bullosa Age Expectancy
The Epidermolysis Bullosa age expectancy can vary significantly depending on the type and severity of the condition. Individuals with milder forms of EB, such as EBS, can have a near-normal lifespan with proper management. However, those with severe forms, like recessive DEB and JEB, may face significant challenges and a reduced lifespan. Factors that can influence Epidermolysis Bullosa age expectancy include:
- The type and severity of EB.
- The presence of complications, such as infections, scarring, and organ involvement.
- The effectiveness of wound care and pain management.
- Access to specialized medical care and support services.
It is important to note that advancements in medical research and treatment options are continually improving the outlook for individuals with EB. Ongoing research into gene therapy and other innovative treatments holds promise for future improvements in Epidermolysis Bullosa age expectancy and quality of life.
Living with Epidermolysis Bullosa
Living with EB presents unique challenges, but with the right support and resources, individuals and their families can navigate these challenges effectively. Key aspects of living with EB include:
- Education and Awareness: Educating family, friends, and caregivers about EB can help create a supportive environment and reduce misunderstandings.
- Support Groups: Joining support groups can provide emotional support, practical advice, and a sense of community. Organizations like the Dystrophic Epidermolysis Bullosa Research Association (DEBRA) offer valuable resources and support.
- Medical Care: Regular medical check-ups and access to specialized care are essential for managing EB effectively. A multidisciplinary team, including dermatologists, geneticists, and physical therapists, can provide comprehensive care.
- Emotional Support: The emotional impact of living with EB can be significant. Counseling and therapy can help individuals and their families cope with the challenges and maintain a positive outlook.
Research and Future Directions
Research into EB is ongoing, with a focus on developing new treatments and improving existing ones. Some of the key areas of research include:
- Gene Therapy: Gene therapy aims to correct the genetic mutations that cause EB. This approach holds promise for potentially curing the condition.
- Stem Cell Therapy: Stem cell therapy involves using stem cells to regenerate damaged skin and promote healing. This approach is still in the experimental stages but shows potential.
- Protein Replacement Therapy: This involves replacing the defective proteins in the skin to improve its integrity and reduce blistering.
- Clinical Trials: Participating in clinical trials can provide access to cutting-edge treatments and contribute to the advancement of medical knowledge.
While these research efforts are promising, it is important to remember that progress takes time. Continued support for research and advocacy is crucial for advancing the field and improving the lives of individuals with EB.
📝 Note: Always consult with healthcare professionals for personalized advice and treatment options.
Epidermolysis Bullosa is a complex and challenging condition that affects individuals and their families in profound ways. Understanding the different types of EB, their symptoms, and the available treatments is essential for managing the condition effectively. While the Epidermolysis Bullosa age expectancy can vary, advancements in medical research and treatment options offer hope for improved outcomes and quality of life. With the right support and resources, individuals with EB can navigate the challenges of this condition and lead fulfilling lives.
Related Terms:
- epidermolysis bullosa treatments
- severe epidermolysis bullosa
- epidermolysis bullosa dystrophica
- epidermolysis bullosa
- epidermolysis bullosa life expectancy average
- epidermolysis bullosa symptoms