Electrocardiograms (ECGs) are crucial tools in cardiology, providing valuable insights into the heart's electrical activity. Understanding abnormal ECG examples is essential for healthcare professionals to diagnose and manage various cardiac conditions effectively. This post delves into the significance of ECGs, common abnormalities, and their clinical implications.
Understanding Electrocardiograms (ECGs)
An ECG is a non-invasive test that records the electrical signals produced by the heart. These signals are translated into waveforms that can be analyzed to detect abnormalities in heart rhythm, conduction, and other cardiac functions. ECGs are widely used in clinical settings to diagnose conditions such as arrhythmias, myocardial infarctions, and electrolyte imbalances.
Common Abnormal ECG Examples
ECGs can reveal a variety of abnormalities, each with its own set of clinical implications. Some of the most common abnormal ECG examples include:
Arrhythmias
Arrhythmias are irregular heart rhythms that can be life-threatening if not managed properly. Common arrhythmias include:
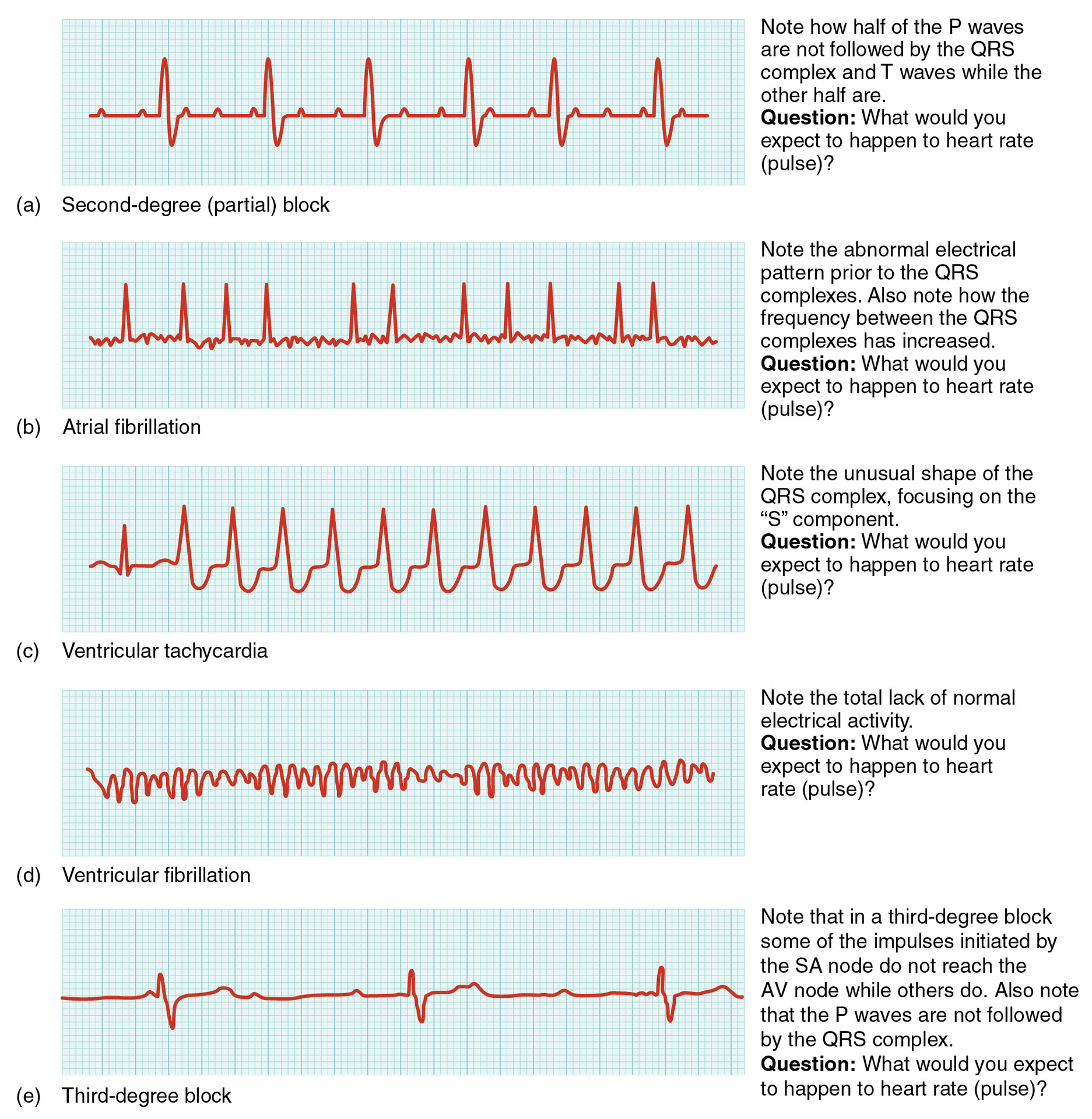
- Atrial Fibrillation (AFib): Characterized by an irregular and often rapid heart rate, AFib can lead to blood clots and stroke.
- Ventricular Tachycardia (VT): A rapid heart rate originating from the ventricles, VT can be life-threatening and requires immediate medical attention.
- Bradycardia: A slow heart rate, often defined as less than 60 beats per minute, can cause symptoms such as dizziness and fatigue.
Conduction Abnormalities
Conduction abnormalities affect the heart’s electrical pathways, leading to issues with the heart’s ability to contract effectively. Examples include:
- Bundle Branch Block (BBB): This condition occurs when the electrical signals are delayed or blocked as they travel through the bundle branches, leading to abnormal QRS complexes.
- Atrioventricular (AV) Block: This refers to a delay or interruption in the conduction of electrical impulses from the atria to the ventricles, which can range from mild to severe.
Myocardial Infarction
Myocardial infarction, commonly known as a heart attack, occurs when blood flow to the heart is blocked, leading to tissue damage. ECG changes in myocardial infarction include:
- ST-Segment Elevation Myocardial Infarction (STEMI): Characterized by elevated ST segments, STEMI requires immediate intervention to restore blood flow.
- Non-ST-Segment Elevation Myocardial Infarction (NSTEMI): This type of heart attack does not show ST-segment elevation but can still cause significant damage.
Electrolyte Imbalances
Electrolyte imbalances, such as those involving potassium, calcium, and magnesium, can significantly affect the heart’s electrical activity. Common ECG changes include:
- Hyperkalemia: Elevated potassium levels can cause peaked T waves and widened QRS complexes.
- Hypokalemia: Low potassium levels can lead to flattened T waves and U waves.
Interpreting Abnormal ECG Examples
Interpreting ECGs requires a systematic approach to identify and understand the abnormalities. Key steps include:
- Rate and Rhythm: Determine the heart rate and identify any irregularities in the rhythm.
- Axis: Assess the electrical axis of the heart to detect any deviations.
- Intervals: Measure the PR, QRS, and QT intervals to identify conduction abnormalities.
- Segments and Waves: Analyze the ST segments and T waves for signs of ischemia or electrolyte imbalances.
🔍 Note: Always compare the ECG findings with the patient's clinical symptoms and medical history for accurate diagnosis.
Clinical Implications of Abnormal ECG Examples
Recognizing abnormal ECG examples is crucial for timely intervention and management. The clinical implications vary depending on the type and severity of the abnormality:
Arrhythmias
Arrhythmias can lead to symptoms such as palpitations, dizziness, and syncope. Severe arrhythmias, like ventricular fibrillation, can be life-threatening and require immediate defibrillation.
Conduction Abnormalities
Conduction abnormalities can impair the heart’s ability to pump blood effectively, leading to symptoms such as fatigue and shortness of breath. Severe conduction abnormalities may require pacemaker implantation.
Myocardial Infarction
Myocardial infarction is a medical emergency that requires immediate intervention to restore blood flow and prevent further damage. Early recognition of ECG changes can save lives.
Electrolyte Imbalances
Electrolyte imbalances can cause cardiac arrhythmias and other complications. Correcting the underlying imbalance is essential for resolving ECG abnormalities and preventing further issues.
Case Studies of Abnormal ECG Examples
To illustrate the clinical significance of abnormal ECG examples, consider the following case studies:
Case Study 1: Atrial Fibrillation
A 65-year-old patient presents with palpitations and shortness of breath. The ECG shows an irregularly irregular rhythm with no distinct P waves, characteristic of atrial fibrillation. The patient is started on anticoagulation therapy to prevent stroke and rate-control medications to manage symptoms.
Case Study 2: ST-Segment Elevation Myocardial Infarction
A 50-year-old patient complains of chest pain radiating to the left arm. The ECG reveals ST-segment elevation in the anterior leads, indicative of a STEMI. The patient is immediately taken for percutaneous coronary intervention (PCI) to restore blood flow and prevent further damage.
Case Study 3: Hyperkalemia
A 70-year-old patient with chronic kidney disease presents with muscle weakness and fatigue. The ECG shows peaked T waves and widened QRS complexes, suggestive of hyperkalemia. The patient is treated with intravenous calcium gluconate to stabilize the cardiac membrane and insulin with glucose to shift potassium into the cells.
Advanced ECG Analysis Techniques
In addition to standard ECG interpretation, advanced techniques can provide deeper insights into cardiac function. These include:
Signal-Averaged ECG
Signal-averaged ECG is used to detect late potentials, which are low-amplitude signals that occur after the QRS complex. These potentials are associated with an increased risk of ventricular arrhythmias.
Holter Monitoring
Holter monitoring involves continuous ECG recording over 24-48 hours, allowing for the detection of intermittent arrhythmias and other transient abnormalities that may not be captured on a standard ECG.
Stress Testing
Stress testing involves monitoring the ECG during exercise or pharmacological stress to assess the heart’s response to increased demand. This can help diagnose conditions such as coronary artery disease and exercise-induced arrhythmias.
Conclusion
Understanding abnormal ECG examples is vital for healthcare professionals to diagnose and manage various cardiac conditions effectively. From arrhythmias to conduction abnormalities and myocardial infarctions, ECGs provide valuable insights into the heart’s electrical activity. By recognizing and interpreting these abnormalities, clinicians can implement timely interventions to improve patient outcomes. Continuous advancements in ECG technology and analysis techniques further enhance our ability to detect and manage cardiac diseases, ensuring better care for patients.
Related Terms:
- abnormal electrocardiogram
- abnormal ecg pictures
- ecg abnormalities chart
- ecg abnormality chart
- abnormal ecg examples with answers
- common ecg abnormalities chart